Silent breast implant rupture: what women should be aware of
In some cases, textured breast implants manufactured using a salt-loss technique may be difficult to assess for rupture on ultrasound. Patients with textured implants such as Allergan, Polytech, or Eurosilicone should inform the implant brand to assist the surgeon in accurately evaluating implant folding, leakage, or rupture.
In addition, it is necessary to monitor breast gland pathology, implant-related conditions, the status of the implant, the fibrous capsule, and the implant pocket, as well as to detect malignancy and other breast abnormalities such as implant rupture, implant folding, and seroma.
MSc., MD Ho Cao Vu has identified several common causes of early breast implant rupture:
- In inframammary fold (IMF) or periareolar breast augmentation, an incision that is too small for the insertion of a large implant (with a large diameter and high projection) may cause damage to the implant during insertion, thereby reducing its longevity over time. In addition, when the implant pocket is revised using blunt dissection (manual exploration of the pocket) while the muscle is relaxed by muscle relaxants, the assessment of pocket size may be inaccurate compared to the state after the effect of the medication has worn off. This may result in insufficient pocket dimensions at the medial border and along the implant base circumference, leading to compression and folding of the implant at the lower pole.
- In transaxillary breast augmentation using blunt dissection techniques, early implant rupture is often associated with two main causes. First, the implant pocket is inadequately created, preventing the implant from being evenly distributed within the pocket. Second, the use of instruments to revise the implant pocket after placement may cause mechanical damage, leading to implant compromise.
- Incorrect implant placement between anatomical planes may subject the implant to compressive forces from the pectoralis major muscle. In blunt dissection techniques, the area most commonly subjected to the greatest pressure is the superomedial quadrant (upper inner quarter) of the implant.
- Some cases of early implant rupture have been observed in patients with a short nipple-to-inframammary fold distance. In these cases, the implant pocket is often created more extensively in the upper pole, causing most of the implant to be displaced superiorly. As a result, the implant is subjected to significant pressure from the pectoralis major muscle, especially in positions that increase muscle tension, such as lying down or during physical activity and exercise. In these situations, the implant pocket may become relatively insufficient, leading to uneven pressure distribution across the implant surface and increasing the risk of implant damage over time.
Signs suggestive of an inadequate implant pocket in patients with a short nipple-to-inframammary fold distance (preoperative measurement < 5 cm): a prominent upper pole fullness, lack of fullness at the lateral border and lower pole; in many cases, the nipple tends to point downward (distinct from breast ptosis).
Early breast implant rupture is one of the potential complications that may occur when the implant size is too large relative to the patient’s anatomical structure. This may necessitate explantation as early as 5–7 years postoperatively, with some cases of rupture occurring as early as 2 years.
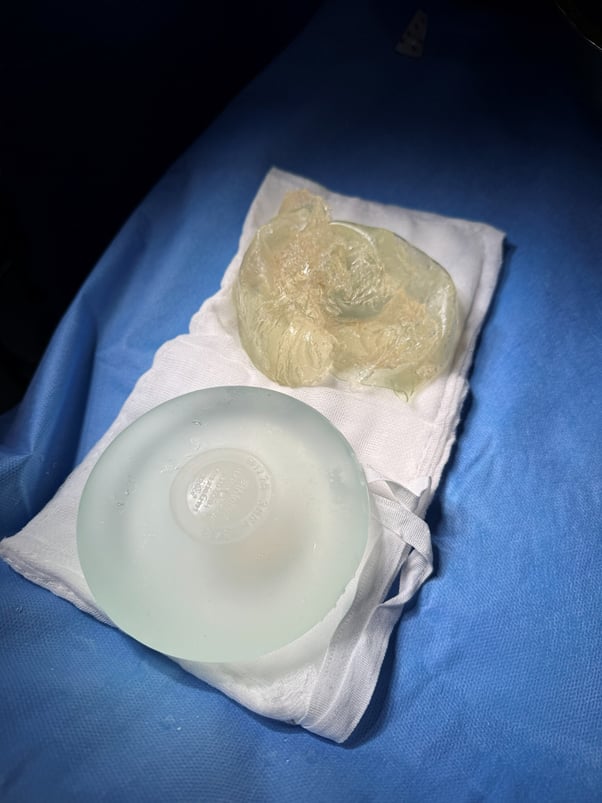
Below are insights from MSc., MD Ho Cao Vu, who has directly managed numerous cases of breast implant rupture, regarding the causes, warning signs, and the procedure for explantation of ruptured breast implants.
Recognizing the risk of early breast implant rupture
After placement into the pocket, the posterior surface of the implant is well expanded and rests against the chest wall. The anterior surface is covered by the pectoralis muscle, breast glandular tissue, and skin. Factors such as an insufficient pocket, oversized implants, incorrect implant positioning, unrelieved pressure from the pectoralis muscle, and capsular contracture may lead to early implant rupture.
Cases in which the implant is not properly positioned can be recognized as follows:
- Progressive widening of the intermammary distance
- Increasing flattening of the upper pole: the distance from the upper pole to the nipple progressively increases
- Excessive upper pole fullness: a shortened nipple-to-inframammary fold distance with superior displacement of the implant
- Lateral displacement of the breast: increased distance from the nipple to the medial pole (especially in the supine position)
Breast implant rupture as early as 2 years after augmentation
Most patients are often only presented with aesthetically pleasing results shortly after surgery or within the first few months, while potential late complications may be overlooked. The following is a case of implant rupture occurring just 2 years after augmentation. Ms. Jun, 36 years old, weighing 45 kg and 157 cm in height, underwent breast augmentation on September 8, 2023. After nearly 2 years, on December 18, 2025, ultrasound examination revealed rupture of the left breast implant. She reported that at her 2-day postoperative follow-up from the previous surgery, her breast shape was symmetrical and satisfactory.
However, after 2 years following breast augmentation, she frequently experienced sharp pain, and the breast shape had changed significantly compared to the early postoperative period: on the right side, implant bottoming out and implant visibility; on the left side, implant rupture. MSc., MD Ho Cao Vu noted that this was the first case he had encountered of breast implant rupture occurring only 2 years after augmentation.
The doctor advised implant explantation, followed by a waiting period of 6 months to 1 year for stabilization before deciding whether to proceed with re-augmentation, in order to reduce the risk of recurrent complications. Patients are advised not to rush. A plan for re-implantation can be prepared if desired.
Dr. Ho Cao Vu further stated that the causes of the four complications observed after 2 years included: improper pocket creation, oversized implants not suitable for the anatomical characteristics of the implant site, and excessive pressure within the pocket, particularly in the upper half of the left breast.
Procedure for explantation of ruptured breast implants using an ultrasonic scalpel
Explantation of ruptured breast implants using an ultrasonic scalpel combined with laryngeal mask anesthesia allows for rapid postoperative recovery with early discharge, without the need for postoperative analgesics or antibiotics (except in cases of Baker grade IV capsular contracture or seroma within the implant pocket). Patients can be discharged 4 hours after surgery.
Step 1: Assess the implant pocket: implant bottoming out, lateral displacement, insufficient pocket, and pressure imbalance (excessive or insufficient pressure)
Step 2: Laryngeal mask anesthesia
Step 3: Use an ultrasonic scalpel to perform dissection into the implant pocket
Step 4: Explant the ruptured breast implant
Step 5: Clean the implant pocket
Step 6: Evaluate the implant pocket for capsular contracture, fibrous bands, and pocket position (over-dissected or under-dissected)
In cases where the patient wishes to undergo re-augmentation with a larger, smaller, or the same implant size, the surgeon must assess the pressure within the pocket. An ultrasonic scalpel is used to expand the implant pocket, and capsulorrhaphy is performed to adjust the pressure within the pocket. A new implant may be inserted, or preparation can be made for a subsequent augmentation procedure. The use of an ultrasonic scalpel for explantation of ruptured breast implants, combined with laryngeal mask anesthesia, is currently highly rated by many patients due to being minimally invasive and allowing rapid recovery. Many patients experience no pain after explantation and are able to resume normal daily activities and return to work 4 hours after surgery.
Risks if ruptured breast implants are not removed
MSc., MD Ho Cao Vu has recorded many cases in which long-standing implant rupture leads to inflammatory reactions between silicone gel and the surrounding tissue within the implant pocket, including papillomatous lesions within the implant pocket, pocket swelling and edema, and chronic inflammation. In some cases, ruptured implants with capsular contracture require evaluation of the appropriate timing for re-implantation. Therefore, early explantation is recommended as soon as rupture is detected.
Tags:





